- ONCOLOGY Vol 14 No 6
- Volume 14
- Issue 6
Update on Low Malignant Potential Ovarian Tumors
Low malignant potential (LMP) ovarian tumors represent a small subset of epithelial ovarian cancers that were first identified 70 years ago but were recognized in a systematic way only within the last 30 years. These lesions
Low malignant potential (LMP) ovarian tumors represent a small subset of epithelial ovarian cancers that were first identified 70 years ago but were recognized in a systematic way only within the last 30 years. These lesions afflict women at a much younger age than invasive ovarian cancer, behave in a more indolent manner, and have a much more favorable prognosis. The management of women with LMP tumors is primarily surgical; adjuvant therapy plays little role in early disease and its use in advanced disease is not well defined. Ongoing investigations are attempting to define prognostic factors that may assist clinicians in the appropriate application of postoperative therapy. [ONCOLOGY 14(6):897-906; 2000]
Epithelial tumors of the ovary account for 60% of all ovarian neoplasms and 80% to 90% of ovarian cancers.[1] Low malignant potential (LMP) tumors of the ovary, also referred to as borderline ovarian tumors, represent a subset of epithelial cancers. These tumors are characterized by the absence of ovarian stromal invasion, and yet they retain the ability to metastasize.
A number of clinical features distinguish LMP ovarian tumors from their invasive counterparts; the most notable of these is the far better outcome of patients with LMP tumors. Clinical and molecular studies continue to refine our understanding of these lesions. This article will review the current management of LMP ovarian tumors.
In 1929, Taylor first recognized the existence of a group of ovarian cancers that were associated with an improved prognosis; he termed these lesions “semimalignant” tumors.[2] In 1961, the International Federation of Gynecology and Obstetrics (FIGO) proposed a classification of ovarian tumors that included LMP lesions; this designation became effective in 1971[3] and was incorporated into the World Health Organization classification in 1973.[4]
Low malignant potential ovarian tumors account for approximately 15% of epithelial ovarian cancers.[5] According to American Cancer Society estimates, almost 4,000 LMP tumors are expected to be diagnosed annually in the United States.[6] The average age of women with LMP ovarian tumors is 49 years, with the highest frequency of cases occurring in the 15- to 29-year age group.[7]
As with invasive ovarian cancer, both oral contraceptive use and lactation lower the risk of developing an LMP tumor, and a history of infertility increases the risk.[8,9] Low malignant potential ovarian tumors may occur in infertile women who have used fertility drugs.[9,10] However, only a small number of such cases have been detected, and limited information is available regarding the specific medications used in these cases; therefore, caution is needed when one is extrapolating from these reports.[9]
The occurrence of pregnancy after treatment for an LMP tumor does not appear to worsen prognosis, nor does the detection of an LMP tumor adversely affect an existing pregnancy.[11]
The use of some deodorizing powders has been associated with an increased risk of developing LMP tumors.[12]
Primary Lesions
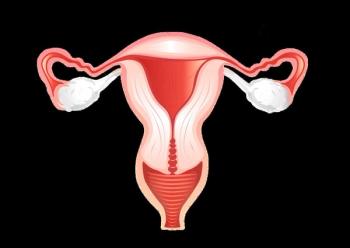
The architecture of LMP ovarian tumors is characterized by solid and cystic areas. Papillary projections often arise within the cystic areas or loculations; surface papillations may also occur. Microscopic features include epithelial proliferation and stratification, nuclear atypia, and mitotic activity, with the sine qua non being the absence of stromal invasion.[1]
Serous and mucinous tumors comprise the vast majority of cases, with endometrioid, clear cell, and Brenner-type tumors also described.[1]
Serous tumors (Figure 1) are bilateral in 25% to 33% of cases. Serous tumors are associated with extraovarian disease much more commonly than are mucinous lesions (30% vs 15%, respectively).
There are two types of mucinous tumors: intestinal and endocervical. The intestinal type has a bilateral incidence of less than 10% but is associated with pseudomyxoma peritonei. The endocervical variant is bilateral in 40% of cases.
Endometrioid LMP tumors can occur in association with hyperplastic or invasive lesions of the endometrium, although extraovarian disease is uncommon. Clear cell and Brenner-type LMP tumors are quite rare.
Low malignant potential ovarian tumors may occur within a background of benign neoplasia and/or in association with areas of invasive disease. Therefore, a thorough sampling of the primary tumor (usually one section for each centimeter of tumor) is critical to the establishment of an accurate diagnosis.
“Microinvasion”-This term has been applied to cases that appear to bridge the definitions of LMP and invasive lesions. Bell and Scully reported a series of cases in which “small foci of stromal invasion,” none larger than 3 mm in greatest dimension, were detected within LMP tumors.[13] Although 2 of the 21 patients studied had advanced disease, all patients who were followed did well.
The authors suggested that the prognosis of cases associated with “microinvasion” is similar to that of other LMP tumors. Although others concur with this finding,[14] the term “microinvasion” should be used with caution until further data are available.
Intraoperative Diagnosis-Intraoperative diagnoses are determined using the well-established technique of frozen section.[15] This technique can accurately identify LMP ovarian tumors. Menzin and colleagues reported that a frozen-section diagnosis of an LMP tumor excluded benign lesions in 94% of cases, although further histologic examination identified foci of invasive disease in 27% of cases.[16]
Pathologists will often use qualifying terms, such as “rule out LMP” and “at least LMP,” in frozen-section reports.[16,17] In the study by Menzin and colleagues, each of the cases that ultimately proved to be benign (6%) were deemed equivocal on frozen-section evaluation.[16] Therefore, a continuing dialog with consultant pathologists is vital for maintaining a clear understanding of clarifying terms that may influence the appropriate application of surgical therapy.
Extraovarian Disease
The peritoneal lesions associated with ovarian LMP tumors are of three types: endosalpingiosis, noninvasive implants, and invasive implants. Endosalpingiosis refers to benign glandular structures similar in appearance to tubal epithelium that can be found on the peritoneum but have also been described at other sites, including lymph nodes.[18] The finding of endosalpingiosis does not appear to hold any prognostic significance and does not signify advanced-stage disease.
Noninvasive implants have the same characteristics as described above for the primary lesions. Invasive implants are distinguished by their irregular borders, as well as by the desmoplastic response of the underlying stroma that is infiltrated by tumor cells.[19]
The extent of a presumed ovarian malignancy may be suggested by preoperative examination and radiologic testing (such as ultrasound or computed tomography [CT]), but the staging of ovarian cancers is determined by an evaluation of samples obtained at the time of surgery (Table 1).[20]
In brief, a thorough exploration of the abdomen and pelvis is undertaken to identify and document disease. This necessitates palpation and visualization of abdominal sites, including the subdiaphragmatic recesses, paracolic gutters, and bowel mesentery. In the absence of grossly disseminated disease, multiple biopsies of the peritoneal surface and retroperitoneum are performed, in addition to the submission of washings for cytologic evaluation.
The staging classification for LMP ovarian tumors follows the criteria defined by FIGO for invasive epithelial ovarian cancer (Table 2).[21] The stage at presentation for LMP ovarian tumors is presented in Table 3.[22]
The survival of patients with LMP ovarian tumors is markedly better than that of patients with invasive epithelial ovarian cancer. The most recent FIGO statistics show overall 5-year disease-related survival rates of 86.2% and 41.6% for women with LMP tumors and invasive lesions, respectively.[7] When extended follow-up has been reported, overall survival rates at 10, 15, and 20 years were 95%, 92%, and 89%, respectively.[23] Table 4 presents the 5- and 20-year survival rates by stage.
Investigators have used CA-125 as a tumor marker to assess therapeutic response among women with invasive epithelial ovarian cancer.[24] Serum CA-125 levels are elevated (greater than 35 U/mL) in approximately 50% of women with early invasive ovarian cancer and approximately 90% of those with advanced disease.
Information regarding women with LMP ovarian tumors is more limited. One recent study of women with LMP tumors noted similar rates of serum CA-125 elevation.[25] Although the presence of CA-125 has been associated most closely with tumors of serous histology, mucinous lesions may also exhibit CA-125 elevation.[25]
Measurement of serum CA-125 is advocated for women found to have LMP ovarian tumors. Whether the CA-125 level is obtained preoperatively or immediately after surgery is a matter of individual physician preference. Should the level be elevated, the test can serve as a marker that may prove useful in the surveillance of such patients.[26] The interpretation of CA-125 may be confounded by the presence of other conditions associated with abnormal values (eg, fibroids, endometriosis, pelvic inflammatory disease).
The factors typically correlated with prognosis for invasive ovarian cancer are also informative for LMP tumors. Younger patients fare better than older ones.[27] Stage of disease correlates with both recurrence risk and survival, as would be expected from the survival data presented above.[7,23,27] The presence of residual disease increases the likelihood of recurrence,[27,28] and appears to confer a survival disadvantage.[27,29] However, reports have described patients with residual and persistent disease who have enjoyed prolonged survival[30,31], as well as those who have experienced spontaneous regression of residual disease.[32,33] Advanced-stage mucinous lesions have also been associated with a worse outcome than serous tumors.[27,34]
Nodal Status-Although the propensity of LMP tumors to involve retroperitoneal lymph nodes is well-documented,[35-38] the prognostic impact of nodal disease is less clear. Despite the presence of nodal disease at diagnosis or at reassessment, prolonged survival has been reported among some patients followed for nearly 11 years.[30,36,37]
Lymph node involvement in association with otherwise localized intraperitoneal disease may confer an elevated risk of recurrence.[38] Therefore, even in the absence of a demonstrable effect on survival, nodal status may provide useful prognostic information.[38]
Peritoneal Implant Histology-The impact of peritoneal implant histology has also received attention. The presence of endosalpingosis does not appear to have a negative effect on prognosis.[19] Additional information is expected to be obtained from the Gynecologic Oncology Group trial (GOG protocol 72) of LMP tumors, in which the outcome of stage I patients with endosalpingosis will be reviewed in a subset analysis.[39]
The predictive value of the “invasiveness” (ie, noninvasive vs invasive) of the peritoneal implants has been reported by some authors[28] and negated by others.[19,40] The most recent reports on this topic have noted that both noninvasive and invasive implants are associated with a relapse in approximately 30% of cases, and that the relapse often is in the form of an invasive low-grade serous carcinoma.[41,42] The median time to relapse was 7.1 years for women with noninvasive implants but 2 years for those with invasive implants.[41,42]
Pseudomyxoma Peritonei or Ovarii-The presence of pseudomyxoma peritonei also increases the risk of recurrence and death.[43-46] The identification of cellular pseudomyxoma ovarii, characterized by the presence of epithelial cells or glandular fragments within pools of mucin infiltrating the ovarian stroma, may represent a manifestation of invasion and, as such, portends an adverse outcome.[47]
DNA Ploidy and S-Phase Fraction-Through the technique of flow cytometry, the prognostic significance of DNA content has been addressed. Several authors have noted the correlation of DNA ploidy with other prognostic factors and have supported its usefulness as a predictor of biological aggressiveness and survival.[48-50] One risk stratification scheme suggested that patients at lowest risk were women under age 40 years with stage I serous or mucinous lesions whose tumors were diploid. Women with the greatest risk of succumbing to their illness were those over age 70 years with aneuploid stage III tumors.[49]
Not all groups have confirmed the power of DNA ploidy or another parameter, S-phase fraction, as accurate predictors,[47,51,52] and the contribution of either test to treatment planning continues to be explored.
Surgery
A total abdominal hysterectomy and bilateral salpingo-oophorectomy (TAH/BSO) represent the cornerstone of the surgical treatment of LMP ovarian tumors. In the absence of gross extraovarian disease, systematic sampling should be undertaken to assess the extent of disease. In the presence of visible metastases, every effort should be made to excise all disease (termed “cytoreduction” or “debulking”). The initial findings, as well as the distribution and extent of residual lesions, should be carefully documented in the operative summary.
Only about half of all patients found to have LMP tumors undergo complete surgical staging.[22] Lin and colleagues noted that gynecologic oncologists had operated on only 10% of the more than 200 women with LMP tumors referred to the M. D. Anderson Cancer Center.[53] These authors found that obstetrician/gynecologists, who operated on 78% of the women in this study, performed comprehensive staging just 9% of the time, and gynecologic oncologists did so in only 50% of cases.[53] Thus, a more consistent approach to the initial surgical management of this condition is warranted.
Appendectomy-Removal of the appendix is often included in the staging procedure for epithelial ovarian cancer, including LMP lesions. The occurrence of synchronous mucinous tumors of the ovary and appendix has been reported.[54-56] Whether the ovarian tumors are secondary or represent dual primary lesions is unclear.[54-56] Nevertheless, because of this association, appendectomy is advocated when a mucinous LMP ovarian tumor is encountered.[43]
Conservative Procedures-When LMP ovarian tumors are identified in premenopausal women, consideration may be given to limiting the extent of surgery. Adnexectomy (or unilateral salpingo-oophorectomy), performed in conjunction with a staging procedure, can provide an acceptable alternative for the woman who has yet to complete childbearing. This management plan is supported by a number of retrospective series,[11,17,23,27,30,34,45,57,58] as well as by prospective trials from the Norwegian Radium Hospital[59] and the GOG.[39]
In the latter report, among 21 patients with confirmed stage I serous LMP ovarian tumors who underwent adnexectomy and were followed without adjuvant therapy, none experienced a recurrence with a median follow-up of 42 months.[39] This result prompted the authors to conclude that adnexectomy and TAH/BSO are equally efficacious among stage I patients, when complete staging has been performed. This sentiment was echoed in the National Institutes of Health (NIH) consensus report on ovarian cancer, in which the option of adnexectomy and staging for premenopausal women wishing to retain childbearing potential was deemed acceptable.[20]
The adequacy of more conservative or conservational procedures, such as ovarian cystectomy, remains the subject of debate. In small retrospective series, cystectomy was associated with only occasional recurrences in the initially involved ovary and had no apparent adverse impact on survival.[30,58]
Lim-Tan and colleagues reported the outcomes of 33 women with stage I and 2 women with stage III disease who underwent cystectomy.[60] Persistence or recurrence occurred in 8% of women with stage I disease and both patients with advanced tumors, although all of the women were alive without evidence of disease at the time of the study report. The authors concluded that tumor close to the resection margins and the removal of multiple cysts predicted recurrence in the ipsilateral ovary.
Unstaged Patients-It is clear that nearly one-third of patients with clinically early (stage I or II) tumors will be found to have more advanced disease if a comprehensive staging procedure is performed.[35,61] Serous tumors are much more likely to be associated with occult metastases than are mucinous tumors.[61] Whether it is beneficial to reexplore women with unstaged tumors has been questioned. If gross residual disease is known or suspected, reoperation to complete cytoreduction is advocated. In the absence of gross disease, however, no clinical benefits of reoperation are evident,[62] and the procedure is not encouraged.[20]
Postoperative Therapy
The use of postoperative therapy for LMP tumors remains the subject of study. A growing body of literature favors the avoidance of adjuvant therapy in patients with stage I lesions. No consensus has been reached for women with more advanced tumors, and the debate continues.
Early Disease-Women with stage I tumors have an excellent prognosis. Both retrospective and prospective studies have failed to demonstrate any survival advantage among this group of patients from the use of adjuvant therapy, whether in the form of radiation (external-beam or intraperitoneal therapy) or chemotherapy (single-agent or combination regimens).[57,59,63,64]
In a prospective study from the GOG, in which comprehensive surgical staging was required, none of the 146 patients with stage I serous LMP tumors experienced a recurrence, despite the absence of postoperative treatment.[39] Although the follow-up in this study was short (median, 42 months), the results support the conclusion that observation alone is appropriate for patients with confirmed stage I LMP ovarian tumors.
Advanced Disease-Several studies have noted that chemotherapy can cause tumor regression, as documented at reassessment surgery.[36,64,65] In fact, in reviewing the literature regarding platinum-based chemotherapy for LMP ovarian tumors, Barakat and colleagues found that 68% of women with microscopic residual disease and 26% of those with macroscopic residual disease were rendered free of disease by chemotherapy.[65]
Tumors associated with invasive implants may have a greater response to chemotherapy than those associated with noninvasive implants.[41,42] These responses, however, have not been accompanied by a demonstrable survival benefit.[36,41,42,64,65]
In this regard, consideration should also be given to the potential side effects of treatment, both acute and chronic. Treatment-related secondary malignancies and death have been reported in women with LMP tumors who were rendered free of disease by chemotherapy.[19,31,36,45]
The determination of selection criteria that could define those women most likely to benefit from adjuvant therapy is of critical import. Whether the prognostic factors discussed above or other parameters will prove to be useful is the subject of ongoing research.
At present, adjuvant therapy is guided by institutional preferences, which often are based on advanced stage, the presence of residual disease and/or invasive implants, or other apparent adverse variables. A consensus, however, remains to be reached.
The importance of LMP ovarian tumors in hereditary ovarian cancer syndromes, most notably, the breast-ovarian cancer syndrome, is unclear. Low malignant potential tumors have been reported in carriers of germ-line mutations in BRCA1.[66] However, in two reports examining the presence of BRCA1 and BRCA2 mutations among women with LMP tumors, evidence for such an association did not emerge.[67,68] Women of Ashkenazi Jewish heritage who develop invasive ovarian cancer harbored germ-line BRCA mutations in 20% to 60% of cases, but a carrier frequency of only 1.6% (1 in 62 cases) was detected among women with LMP tumors.[67,68]
Given that the hereditary implications of LMP tumors require further clarification, recommendations regarding genetic counseling should be individualized.
The use of hormone replacement therapy has not yet undergone systematic analysis among women with LMP ovarian tumors.[43] The young age at diagnosis and favorable long-term outcome of these tumors mandate consideration of the risks and benefits of hormone replacement therapy.
The well-documented risks of osteoporosis and cardiovascular disease can be positively affected by HRT, as may a woman’s overall quality of life. For these reasons, women with LMP ovarian tumors should be offered hormone replacement therapy, unless other issues mitigate against its use.[26]
Low malignant potential ovarian tumors remain a fertile area of investigation. Efforts to ensure a consistent surgical approach to this disease are needed, as are methods to identify women who will benefit most from adjuvant therapy.
References:
1. Russell P: Surface epithelial-stromal tumors of the ovary, in Kurman RJ (ed): Blaustein’s Pathology of the Female Genital Tract, pp 705-782. New York, Springer-Verlag, 1994.
2. Taylor HC: Malignant and semimalignant tumors of the ovary. Surg Obstet Gynecol 48:204-230, 1929.
3. International Federation of Gynecology and Obstetrics: Classification and staging of malignant tumors in the female pelvis. Acta Obstet Gynecol Scand 50:1-7, 1971.
4. Serov SF, Scully RE, Solvin LH: Histological typing of ovarian tumors, in International Histological Classification of Tumors, no. 9, pp 37-38. Geneva, World Health Organization, 1973.
5. Colgan TJ, Norris HJ: Ovarian epithelial tumors of low malignant potential: A review. Int J Gynecol Pathol 1:367-382, 1983.
6. Landis SH, Murray T, Bolden S, et al: Cancer statistics, 1999. CA Cancer J Clin 49:8-31, 1999.
7. Pecorelli S, Odicino F, Maisoneuve P, et al: Carcinoma of the ovary. J Epidemiol Biostat 3:75-102, 1998.
8. Harlow BL, Weiss NS, Roth GJ, et al: Case-control study of borderline ovarian tumors: Reproductive history and exposure to exogenous female hormones. Cancer Res 48:5849-5852, 1988.
9. Parazzini F, Negri E, La Vecchia C, et al: Treatment for fertility and risk of ovarian tumors of borderline malignancy. Gynecol Oncol 68:226-228, 1998.
10. Harris R, Whittemore AS, Intyre J: Collaborative ovarian cancer group: Characteristics relating to ovarian cancer risk: Collaborative analysis of 12 US case-control studies. Am J Epidemiol 136:1184-1203, 1992.
11. Gotlieb WH, Flikker S, Davidson D, et al: Borderline tumors of the ovary: Fertility treatment, conservative management, and pregnancy outcome. Cancer 82:141-146, 1998.
12. Harlow BL, Weiss NS: A case-control study of borderline ovarian tumors: The influence of perineal exposure to talc. Am J Epidemiol 130:390-394, 1989.
13. Bell DA, Scully RE: Ovarian serous borderline tumors with stromal microinvasion: A report of 21 cases. Hum Pathol 21:397-403, 1990.
14. Kennedy AW, Hart WR: Ovarian papillary serous tumors of low malignant potential (serous borderline tumors): A long-term follow-up study, including patients with microinvasion, lymph node metastases, and transformation to invasive serous carcinoma. Cancer 78:278-286, 1996.
15. Obiakor I, Maiman M, Mittal K, et al: The accuracy of frozen section in the diagnosis of ovarian neoplasms. Gynecol Oncol 43:61-63, 1991.
16. Menzin AW, Rubin SC, Noumoff JS, et al: The accuracy of a frozen section diagnosis of borderline ovarian malignancy. Gynecol Oncol 59:183-185, 1995.
17. Robinson WR, Curtin JP, Morrow CP: Operative staging and conservative surgery in the management of low malignant potential ovarian tumors. Int J Gynecol Cancer 2:113-118, 1992.
18. Clement PB: Diseases of the peritoneum, in Kurman RJ (ed): Blaustein’s Pathology of the Female Genital Tract, pp 647-703. New York, Springer-Verlag, 1994.
19. Gershenson DM, Silva EG: Serous ovarian tumors of low malignant potential with peritoneal implants. Cancer 65:578-585, 1990.
20. NIH Consensus Development Panel on Ovarian Cancer: Ovarian cancer: Screening, treatment, and follow-up. JAMA 273:491-497, 1995.
21. Staging announcement: FIGO Staging Committee. Gynecol Oncol 25:383-385, 1986.
22. Link CJ Jr, Reed E, Sarosy G, et al: Borderline ovarian tumors. Am J Med 101:217-225, 1996.
23. Leake JF, Currie JL, Rosenshein NB, et al: Long-term follow-up of serous ovarian tumors of low malignant potential. Gynecol Oncol 47:150-158, 1992.
24. Evans AC, Berchuck A: Tumor markers, in Hoskins WJ, Perez CA, Young RC (eds): Principles and Practice of Gynecologic Oncology, pp 177-195. Philadelphia, Lippincott-Raven, 1997.
25. Rice LW, Lage JM, Berkowitz RS, et al: Preoperative serum CA-125 levels in borderline tumors of the ovary. Gynecol Oncol 46:226-229, 1992.
26. Trope C, Kaern J: Management of borderline tumors of the ovary: State of the art. Semin Oncol 25:372-380, 1998.
27. Kaern J, Trope CG, Abeler VM: A retrospective study of 370 borderline tumors of the ovary treated at the Norwegian Radium Hospital from 1970 to 1982: A review of clinicopathologic features and treatment modalities. Cancer 71:1810-1820, 1993.
28. Bell DA, Weinstock MA, Scully RE: Peritoneal implants of ovarian serous borderline tumors: Histologic features and prognosis. Cancer 62:2212-2222, 1988.
29. Leake JF: Tumors of low malignant potential. Curr Opin Obstet Gynecol 4:81-85, 1992.
30. Rice LW, Berkowitz RS, Mark SD, et al: Epithelial ovarian tumors of borderline malignancy. Gynecol Oncol 39:195-198, 1990.
31. O’Quinn AG, Hannigan EV: Epithelial ovarian neoplasms of low malignant potential. Gynecol Oncol 21:177-185, 1985.
32. Taylor HC, Wilson EA: Spontaneous regression of peritoneal implantations from ovarian papillary cystadenoma. Am J Cancer 16:1305-1325, 1932.
33. Gaudrault GL: Papillary carcinoma of the ovary: Report of a case with prolonged dormancy and spontaneous regression of metastases. N Engl J Med 264:398, 1961.
34. Nikrui N: Survey of the clinical behavior of patients with borderline epithelial tumors of the ovary. Gynecol Oncol 12:107-119, 1981.
35. Yazigi R, Sandstad J, Munoz AK: Primary staging in ovarian tumors of low malignant potential. Gynecol Oncol 31:402-408, 1988.
36. Sutton GS, Bundy BN, Omura GA, et al: Stage III ovarian tumors of low malignant potential treated with cisplatin combination therapy (a Gynecologic Oncology Group study). Gynecol Oncol 41:230-233, 1991.
37. Tan LK, Flynn SD, Carcangiu ML: Ovarian serous borderline tumors with lymph node involvement: Clinicopathologic and DNA content study of seven cases and review of the literature. Am J Surg Pathol 18:904-912, 1994.
38. Leake JF, Rader JS, Woodruff JD, et al: Retroperitoneal lymphatic involvement with epithelial ovarian tumors of low malignant potential. Gynecol Oncol 42:124-130, 1991.
39. Barnhill DR, Kurman RJ, Brady MF, et al: Preliminary analysis of the behavior of stage I ovarian serous tumors of low malignant potential: A Gynecologic Oncology Group study. J Clin Oncol 13:2752-2756, 1995.
40. Michael H, Roth LM: Invasive and noninvasive implants in ovarian serous tumors of low malignant potential. Cancer 57:1240-1247, 1986.
41. Gershenson DM, Silva EG, Tortolero-Luna G, et al: Serous borderline tumors of the ovary with noninvasive peritoneal implants. Cancer 83:2157-2163, 1998.
42. Gershenson DM, Silva EG, Levy L, et al: Ovarian serous borderline tumors with invasive peritoneal implants. Cancer 82:1096-1103, 1998.
43. Trimble CL, Trimble EL: Management of epithelial ovarian tumors of low malignant potential. Gynecol Oncol 55:S52-S61, 1994.
44. Nakashima N, Nagasoka T, Oiwa N, et al: Ovarian epithelial tumors of borderline malignancy in Japan. Gynecol Oncol 38:90-98, 1990.
45. Casey AC, Bell DA, Lage JM, et al: Epithelial ovarian tumors of borderline malignancy: Long-term follow-up. Gynecol Oncol 50:316-322, 1993.
46. Kliman L, Rome RM, Fortune DW: Low malignant potential tumors of the ovary: A study of 76 cases. Obstet Gynecol 68:338-344, 1986.
47. Guerrieri C, Hogberg T, Wingren S, et al: Mucinous borderline and malignant tumors of the ovary: A clinicopathologic and DNA ploidy study of 92 cases. Cancer 74:2329-2340, 1994.
48. Kaern J, Trope C, Kjorstad KE, et al: Cellular DNA content as a new prognostic tool in patients with borderline tumors of the ovary. Gynecol Oncol 38:452-457, 1990.
49. Kaern J, Trope CG, Kristensen GB, et al: DNA ploidy: The most important prognostic factor in patients with borderline tumors of the ovary. Int J Gynecol Cancer 3:349-358, 1993.
50. Friedlander ML, Russell P, Taylor IW, et al: Flow cytometric analysis of cellular DNA content as an adjunct to the diagnosis of ovarian tumors of borderline malignancy. Pathology 16:301-306, 1984.
51. Demirel D, Laucirica R, Fishman A, et al: Ovarian tumors of low malignant potential: Correlation of DNA index and S-phase fraction with histopathologic grade and clinical outcome. Cancer 77:1494-1500, 1996.
52. Seidman JD, Norris HJ, Griffin JL, et al: DNA flow cytometric analysis of serous ovarian tumors of low malignant potential. Cancer 71:3947-3951, 1993.
53. Lin PS, Gershenson DM, Bevers MW, et al: The current status of surgical staging of ovarian serous borderline tumors. Cancer 85:905-911, 1999.
54. Young RH, Gilks B, Scully RE: Mucinous tumors or the appendix associated with mucinous tumors of the ovary and pseudomyxoma peritonei: A clinicopathologic analysis of 22 cases supporting an origin in the appendix. Am J Surg Pathol 15:415-429, 1991.
55. Prayson RA, Hart WR, Petras RE: Pseudomyxoma peritonei: A clinicopathologic study of 19 cases with emphasis on site of origin and nature of associated ovarian tumors. Am J Surg Pathol 18:591-603, 1994.
56. Seidman JD, Elsayed AM, Sobin LH, et al: Association of mucinous tumors of the ovary and appendix: A clinicopathologic study of 25 cases. Am J Surg Pathol 17:22-34, 1993.
57. Chambers JT, Merino MJ, Kohorn EI, et al: Borderline ovarian tumors. Am J Obstet Gynecol 159:1088-1094, 1988.
58. Tazelaar HD, Bostwick DG, Ballon SC, et al: Conservative treatment of borderline ovarian tumors. Obstet Gynecol 66:417-422, 1985.
59. Trope C, Kaern J, Vergote B, et al: Are borderline tumors of the ovary overtreated both surgically and systemically? A review of four prospective randomized trials including 253 patients with borderline tumors. Gynecol Oncol 51:236-243, 1993.
60. Lim-Tan SK, Cajigas HE, Scully RE: Ovarian cystectomy for serous borderline tumors: A follow-up study of 35 cases. Obstet Gynecol 72:775-780, 1988.
61. Snider DD, Stuart GCE, Nation JG, et al: Evaluation of surgical staging in stage I low malignant potential ovarian tumors. Gynecol Oncol 40:129-132, 1991.
62. Stier EA, Barakat RR, Curtin JP, et al: Laparotomy to complete staging of presumed early ovarian cancer. Obstet Gynecol 87:737-740, 1996.
63. Creasman WT, Park R, Norris H, et al: Stage I borderline ovarian tumors. Obstet Gynecol 59:93-96, 1982.
64. Fort MG, Pierce VK, Saigo PE, et al: Evidence for the efficacy of adjuvant therapy in epithelial ovarian tumors of low malignant potential. Gynecol Oncol 32:269-272, 1989.
65. Barakat RR, Benjamin I, Lewis JL Jr, et al: Platinum-based chemotherapy for advanced-stage serous ovarian carcinoma of low malignant potential. Gynecol Oncol 59:390-393, 1995.
66. Rubin SC, Benjamin I, Behbakht K, et al: Clinical and pathological features of ovarian cancer in women with germ-line mutations of BRCA1. N Engl J Med 335:1413-1416, 1996.
67. Gotlieb WH, Friedman E, Bruchim R et al: Rates of Jewish ancestral mutations in BRCA1 and BRCA2 in borderline ovarian tumors. J Natl Cancer Inst 90:995-1000, 1998.
68. Lu KH, Cramer DW, Muto MG, et al: A population-based study of BRCA1 and BRCA2 mutations in Jewish women with epithelial ovarian cancer. Obstet Gynecol 93:34-37, 1999.
Articles in this issue
almost 26 years ago
Purine Nucleoside Analogs in Indolent Non-Hodgkin’s Lymphomaalmost 26 years ago
New Website Addresses Epidermal Growth Factor Receptors in Cancer Therapyalmost 26 years ago
Common p53 Gene Test Helps Predict Cancer Recurrence in Mastectomy Patientsalmost 26 years ago
New Treatment Guidelines Available for Colon and Rectal Cancer Patientsalmost 26 years ago
Breath Test Identifies Patients Who Should Get Lower Chemotherapy Dosesalmost 26 years ago
3D CRT More Cost-Effective Than Conventional RT for Prostate CancerNewsletter
Stay up to date on recent advances in the multidisciplinary approach to cancer.