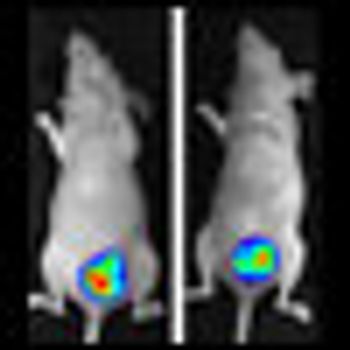
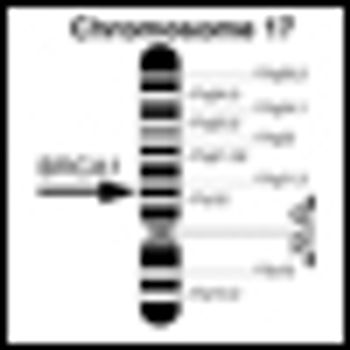
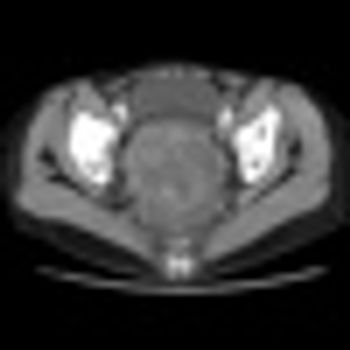
Coffee is emerging as a protective agent against a number of diseases, including cancer. A study published last week shows that women who drank more than four cups of coffee per day cut their risk of endometrial cancer by 25% compared with those who drank less than one cup per day.