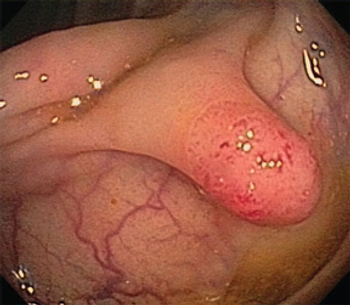
Two French studies have shown that screening for colorectal cancer with fecal occult blood tests can be very effective, according to results presented at the ESMO 2014 Congress.

Your AI-Trained Oncology Knowledge Connection!


Two French studies have shown that screening for colorectal cancer with fecal occult blood tests can be very effective, according to results presented at the ESMO 2014 Congress.
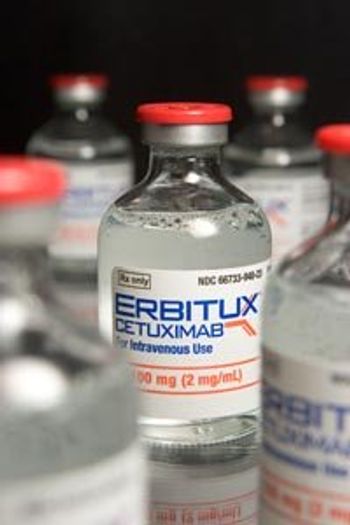
Adding cetuximab (Erbitux) to the standard first-line FOLFIRI chemotherapy regimen results in longer overall survival in metastatic colorectal cancer patients.
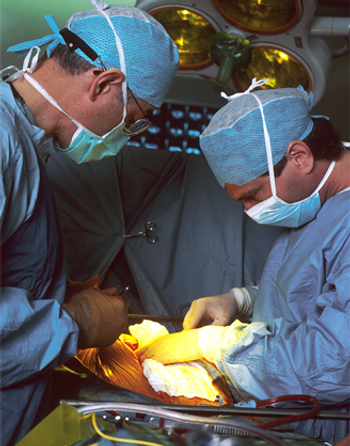
A systematic, best-practice approach to colorectal surgery can decrease the risk of surgical site infections, according to a new study.

This article discusses features that predict local recurrence and distant metastasis in rectal cancer, and how to use MRI to guide treatment decisions.

There are a number of clinicopathologic variables that predict outcome in rectal cancer. In the era of postoperative chemoradiation treatment, these were more easily identified and were used to help select patients for adjuvant therapy.

The authors propose that current policies regarding the use of chemoradiotherapy or short-course preoperative radiotherapy have resulted in an approach to rectal cancer management that often represents overtreatment, with significant loss of quality of life for patients.

Yesterday, the US Food and Drug Administration (FDA) approved the first DNA-based stool sample screening test for colorectal cancer.

A comprehensive analysis of studies and trials suggests the cancer prevention benefits of a daily aspirin for at least 5 years outweigh the potential harms.


Rectal cancer management is becoming increasingly complex. There is increasing recognition of the potential to avoid routine chemoradiotherapy, as excellent results can be achieved with a more selective approach.

Although the current standard treatment for patients with locally advanced rectal cancer is preoperative chemoradiotherapy followed by total mesorectal excision, concerns have been raised over the functional sequelae and possible overtreatment of rectal cancer patients.

In this article, we review risks and benefits of the standard treatment approach for rectal cancer and compare standard treatment with alternative methods aimed at rectal preservation.

Colorectal cancer patients with higher levels of plasma vitamin D have better survival outcomes, according to a new prospective study.

Age is a prognostic factor for both overall survival and progression-free survival among patients diagnosed with metastatic colorectal cancer, according to the results of a study.

Consuming more than two servings of fish each week can reduce a person’s risk for recurrence of colorectal cancer, according to the results of a cross-sectional multinational study.

The landscape of cancer therapy is shifting from traditional cytotoxic chemotherapy towards targeted therapy with agents like tyrosine kinase inhibitors and monoclonal antibodies. However, these newer agents remain costly, and traditional chemotherapy remains the backbone for treating most malignancies.
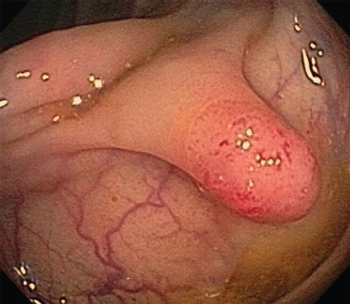
Methods of screening for colorectal cancer are estimated to have prevented between a quarter of a million to a half a million colorectal cancers, according to a recently published study.

Colorectal cancer screening should be considered in unscreened patients aged 75 years or older, especially those with no comorbid conditions, according to a new study.

First-line treatment with chemotherapy plus either bevacizumab or cetuximab resulted in equally effective outcomes for patients with metastatic colorectal cancer.

Maintenance treatment with capecitabine and bevacizumab after 6 cycles of CAPOX B is an effective treatment in patients with metastatic colorectal cancer, according to the final results of the CAIRO3 study.

Exposure to a preference-based mail and telephone navigation intervention increased colorectal cancer (CRC) screening adherence compared to a standard mailed intervention among African Americans.
The role of oxaliplatin in early-stage rectal cancer may still be unclear, according to the differing disease-free survival results from two studies presented at the 2014 ASCO Annual Meeting.

Treatment with oxaliplatin-containing FOLFOX significantly improved the 3-year disease-free survival of select patients with curatively resected rectal cancer compared with treatment with 5-fluorouracil/leucovorin.

As part of our coverage of the 2014 ASCO Annual Meeting, we discuss some of the colorectal cancer research that is expected to be presented at the meeting.

Urban environments had a higher density of colorectal care providers including gastroenterologists, general surgeons, and radiations oncologists compared with rural environments, according to the results of a recent retrospective study.